A week after our twins were born, I noticed something not quite right about my daughter's eye. There was something behind the pupil - a gray fuzzy something. I didn't know what it was, but suddenly I was worried about all kinds of words that end in the letters -oma (e.g. retinoblastoma.) Was it a cancer of some kind?
Fortunately, a visit from the opthalmologist revealed that our daughter had a cataract and nothing more serious than that. I quickly searched for information on cataracts, but didn't find a single account with all the information a worried parent would want.. After some research as well as conversations with the doctor who treated my daughter's eye, I put together this piece on congenital cataracts in terms that a layman can understand.
You may wish to review a cross-section of the eye.
'Congenital' simply means 'present at birth', so a congenital cataract is a cataract that a baby is born with. Somewhere between 500 and 1500 babies are born with congenital cataracts each year in the U.S. - somewhere around 3 babies in 10,000. Rates in developing nations may be higher.
Many congenital cataracts are hereditary. If there is no history in the family, they can be caused by a hereditable mutation in the infant - the infant's future children may be at risk even if there is no previous family history.
 It's usually easier to tell if he does not. When a
pediatrician looks into a child's eye, she's looking for "red
reflex". This is something most of us will be familiar with as "red
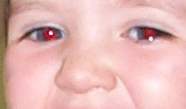
eye" when taking a flash picture. Here is a picture of my toddler's
eyes, you'll notice both are quite red. This is a healthy sign - she
has no cataracts, unlike her younger sister.
It's usually easier to tell if he does not. When a
pediatrician looks into a child's eye, she's looking for "red
reflex". This is something most of us will be familiar with as "red
eye" when taking a flash picture. Here is a picture of my toddler's
eyes, you'll notice both are quite red. This is a healthy sign - she
has no cataracts, unlike her younger sister.
In the case of a cataract, the eye will not reflect red light like this. If you notice that anyone in your family suddenly stops having red eyes (or has only one red eye) in flash pictures, have them see an eye doctor soon.
In some cases, a cataract may be visible to the naked eye, as was the case with my daughter. Upon inspection, the pediatrician noted a lack of red reflex, and an opthalmologist later gave the diagnosis.
If the cataract is visually significant, meaning it is large enough or in a sensitive enough location to block light from the retina, the vision of the eye is permanently threatened. This is not through any damage to the eye tissue, but rather through allowing the vision centers of the brain to languish. Unused, this portion of the brain will eventually give up on vision, resulting in permanent loss of vision in that eye.
Interestingly, this problem is worse in cases where only one eye has a cataract. This seems to be an extreme form of amblyopia (lazy eye). I suspect that the presence of a good eye causes the brain's visual centers to develop, where the absense of any good eye gives some amount of time for correction to be made.
For cataracts that impair vision however, the cataract must be removed in order for light to hit the retina and start training the vision centers of the brain. The only way to accomplish this is to remove the lens entirely. For infants the procedure seems to be a kind of vacuum aspiration, where a very small incision in the eye is made. Recovery is quick - in my daughter's case, she had a protective patch on for only one week.
Timing is critical - especially in cases where only one eye is affected. Surgery before two months of age provides the best chance of good vision - after that, the risk of vision loss or degradation is greater.
Without a lens, the eye is hopelessly farsighted. Corrective glasses are both impractical for infants as well as useless for treating this condition due to focal length problems, so the remaining options are a contact lens or an implanted lens (intraocular lens).
Implantation of intraocular lenses in infants is controversial. First, it is difficult to calculate the appropriate strength of lens required, especially since the eye is still growing. Second, intraocular lenses do not accomodate (i.e. change focal length - for example when you look at something close in, your lens changes focal length.) These two factors mean you'll need corrective lenses anyway.
Our opthalmologist is in the camp that believes the intraocular lens is not helpful, so we now have a 29 diopter contact lens in our daughter's right eye. Changing a contact lens in an infant is an interesting challenge!
If no lens was implanted at the time of lens extraction, one can be implanted later after the eye has stopped growing, but this involves another set of surgical risks to be balanced against the potential benefits.
Because of the trauma of the surgery, it is possible that the pupil of the affected eye will not be the same size as the other eye.
The strong corrective contact lens will never be a perfect replacement for a natural lens - thus, the affected eye will not be as good as an unaffected eye, for those with only one affected eye. This leads to a risk of amblyopia, so patching the good eye for part of the child's awake time is required, probably for many years.